1266 Results found.

Midwest Health Plan Earns NCQA Accreditation
THE CLIENT
A managed care health system serving the comprehensive needs of communities and offering care delivery sites across the Midwest.
THE CHALLENGE
The client wanted to expand its reach by offering its Marketplace product in in a nearby state. T he state requires either National Committee for Quality Assurance (NCQA) accreditation or Centers for Medicare and Medicaid Services (CMS) approval to determine network adequacy and allow plans to operate in the state. The client, already established with HMA in other states, reached out to secure our services to help them with the accreditation process.
While NCQA accreditation is never easy, this process was complicated by several factors including a six-month timeline in order to start processing requests during the open enrollment period, as well as a complex company structure.
APPROACH
Working on-site, HMA’s experts assembled a team from the client’s staff to assist with the accreditation process and completed a second-level review of every document as they readied the accreditation submission. After submission, HMA consultants helped the team answer two rounds of complex questions in response to requests from NCQA.
The biggest challenges were questions regarding the company’s organizational structure because the plan operates under different names in different states. Multiple-state accreditation is a challenge to explain to NCQA, but HMA’s seasoned experts were able to create a very clear document and explanation that showed the organizational structure and sole ownership of the health plan. This was crucial because it was a non-typical issue and questions needed to be answered in a satisfactory manner in order to ensure accreditation and the ability to sell the plan’s product during open enrollment for 2020.
In addition, in order to ensure the accreditation was secured in time, our team was able to obtain an expedited decision from NCQA. Preparing for accreditation is usually a year-long process, but the team was able to complete the process and secure accreditation in less than six months.
RESULTS
The client was granted interim accreditation status on November 15, 2019, in time for the plan to enter the marketplace for open enrollment. Coming up just two points short of a perfect score, the plan reached its goal of opening services in the state.
In addition to helping the client reach its goal, HMA experts continue to work with the company to tailor and implement a Survey Ready Model to ensure they are prepared for the next accreditation cycle. HMA also is providing accreditation services to the client in two additional states.
The company president and chief executive officer said accreditation would not have been possible without HMA’s expertise and guidance.

West Virginia releases Medicaid managed care RFP
This week, our In Focus section reviews the West Virginia Mountain Health Trust request for proposals (RFP) released by the West Virginia Department of Administration (DOA) for the Department for Health and Human Resources (DHHR) on December 17, 2019. Mountain Health Trust (MHT) is the statewide physical and behavioral Medicaid managed care program. West Virginia will award contracts, worth over $1.5 billion, to three managed care organizations (MCOs), with implementation beginning July 1, 2020.

Hospital Charges and Reimbursement for Medicines: Analysis of Cost-to-Charge Ratios
This report is an update to a previous report examining hospital markups for separately paid drugs. Our prior analysis examined hospital charges and reimbursement for 20 drugs and found that hospitals marked up charges for those drugs, on average, 487 percent of their acquisition cost. We also found that hospitals receive 252 percent of estimated hospital acquisition cost from commercial payers. Hospital reimbursement data was obtained from the Magellan Rx Management Medical Pharmacy Trend Report™: 2016 Seventh Edition (the Magellan report) and charges were calculated from Medicare claims data. For more information, please refer to our prior analysis.

Michigan Medicaid Managed Care Results Announced
In previous editions of The Michigan Update (most recently in August) we have reported on the Michigan Department of Health and Human Services’ (MDHHS) release of a Request for Proposals (RFP) to re-procure its Medicaid managed care contracts. The RFP was released in early May with bidder responses due in early August. This procurement is for at least five years, with the possibility of up to three one-year extensions. The total cost of the procurement for five years is estimated to be $35 billion. On October 13, 2015 the State of Michigan announced the much anticipated results of the re-procurement.
Since the prices paid to the contracted HMOs are set by the state, the health plan selection was based solely on technical scores. The HMOs were required to bid on entire regions, which were configured differently than in the past. The reconfiguration required a number of the HMOs to expand their service areas to meet the “entire region” requirement. The new regional configuration appears in the map below:
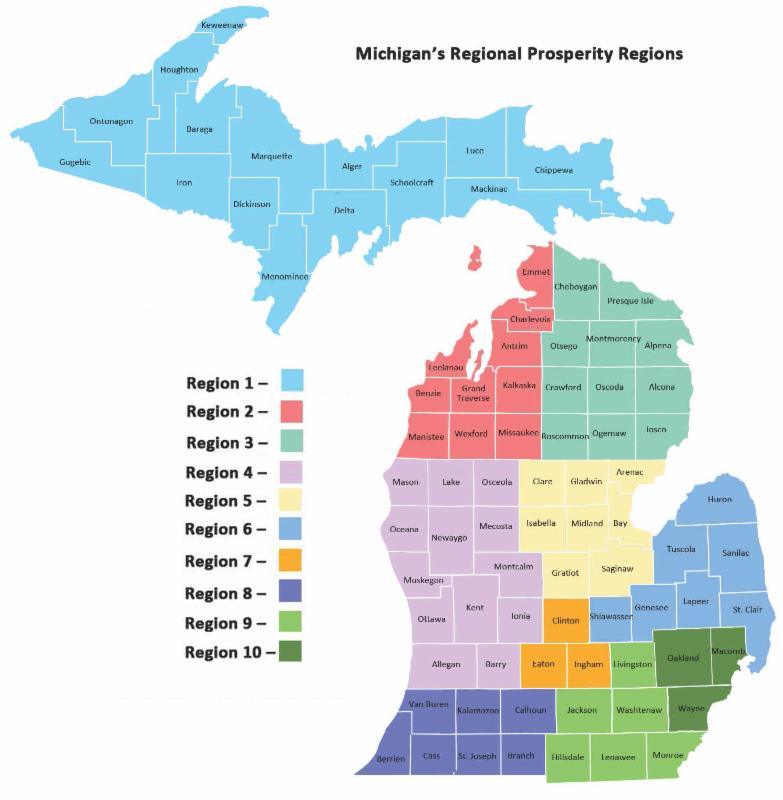
Note: Region 2 and Region 3 were required to be bid together.
The RFP included a proposed number of HMOs that would be awarded contracts for each of these regions. To minimize disruptions for Medicaid enrollees, in each region (other than the Upper Peninsula) the number of plans selected was one more than the proposed maximum number of awards for that region. Proposals from the HMOs were evaluated based on demonstrated competencies and also statements of their proposed approaches to many new initiatives related to population health, care management, behavioral health integration, patient-centered medical homes, health information technology and payment reform.
Not every HMO was successful in each region for which it submitted a bid. Two plans were not successful in any region. One is Sparrow PHP, which is an incumbent plan in Region 7. The other is MI Complete Health (Centene/Fidelis SecureCare) which is not currently a Medicaid plan in any part of the state but does have an Integrated Care Organization contract to serve dual Medicare/Medicaid enrollees in Macomb and Wayne counties as part of Michigan’s dual eligible demonstration.
The following table indicates the regions for which each bidding HMO was and was not successful. In addition, the numerical values show the rank of that plan based on their evaluation scores among the successful bidders for each region. If an HMO is a current contractor for all counties in a region, their result is shaded green. If the HMO is a current contractor for some but not all counties in a region, their result is shaded yellow. The number of Medicaid enrollees currently served in each of the regions, eligible through both “traditional” Medicaid and the Healthy Michigan Plan, appear in the bottom row on the table; across all regions, this is more than 1.6 million Medicaid enrollees.
Technical Evaluation Results
|
|
Region 1
|
Region 2
|
Region 3
|
Region 4
|
Region 5
|
Region 6
| Region 6 |
Region 8
|
Region 9
|
Region 10
|
|
Aetna Better Health
(CoventryCares)
|
|
|
|
|
No
|
|
|
Yes – 4
|
Yes – 4
|
Yes – 7
|
|
Blue Cross Complete
|
|
|
|
Yes – 3
|
|
Yes – 5
|
Yes – 3
|
|
Yes – 3
|
Yes – 5
|
|
HAP Midwest Health Plan
|
|
|
|
|
|
Yes – 6
|
|
|
No
|
No
|
|
Harbor Health
Plan
|
|
|
|
|
|
|
|
|
|
Yes – 8
|
|
McLaren Health
Plan
|
|
Yes – 3
|
Yes – 3
|
Yes – 4
|
Yes – 3
|
Yes – 3
|
Yes – 2
|
Yes – 3
|
Yes – 6
|
Yes – 4
|
|
Meridian Health Plan of MI
|
|
Yes – 1
|
Yes – 4
|
Yes – 5
|
Yes – 2
|
Yes – 4
|
No
|
Yes – 5
|
Yes – 5
|
Yes – 3
|
|
MI Complete Health
(Centene/Fidelis)
|
|
|
|
|
|
|
|
|
No
|
No
|
|
Molina Healthcare
of MI
|
|
Yes – 4
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
|
Priority Health Choice
|
|
No
|
No
|
