This week, our In Focus comes from HMA Vice President Kathleen Nolan and Managing Principal Jon Blum. On March 13, 2020, President Trump declared a national emergency due to the rapid spread of COVID-19 virus. This declaration provides Health and Human Services (HHS) and the Centers of Medicare and Medicaid Services (CMS) new abilities to waive Medicare and Medicaid regulatory requirements to help health care providers, health plans and other stakeholders respond to immediate needs of their patients and communities. In the past, HHS and CMS have solicited requests for relief needs from states, local providers and trade associations, among other stakeholders. Health care providers, health plans and others should continue to monitor policy announcements from HHS and CMS and work with their states and trade associations to identify potential areas of need for requested regulatory relief.
323 Results found.

Medicaid managed care enrollment update – Q4 2019
This week, our In Focus section reviews recent Medicaid enrollment trends in capitated, risk-based managed care in 29 states.[1] Many state Medicaid agencies post monthly enrollment figures by health plan for their Medicaid managed care population to their websites. This data allows for the timeliest analysis of enrollment trends across states and managed care organizations. All 29 states highlighted in this review have released monthly Medicaid managed care enrollment data into the fourth quarter (Q4) of 2019. This report reflects the most recent data posted. HMA has made the following observations related to the enrollment data shown on Table 1 (below):

Former Illinois Medicaid director named COO of ������
������ (HMA) announced today that Douglas (Doug) L. Elwell, who most recently served as Medicaid director for the State of Illinois in the Department of Healthcare and Family Services, has joined the firm as chief operating officer (COO).

Medicaid expansion in Missouri: economic implications and insights from Arkansas, Indiana, and Ohio
This week, our In Focus section covers the report, Medicaid Expansion in Missouri – Economic Implications for Missouri and Interviews Reflecting Arkansas, Indiana, and Ohio Experiences, prepared by HMA Medicaid Market Solutions (MMS) Managing Director Matt Powers and Managing Principal Sharon Silow-Carroll, and Independent Health Policy Consultant Jack Meyer. ������ (HMA) conducted a targeted analysis of the likely economic impact of an ACA Medicaid Expansion in Missouri, with an emphasis on the effects on the state budget. The report was commissioned by the Missouri Hospital Association and Missouri Primary Care Association and released in partnership with stakeholders from the health care community in January 2020.

CMS Unveils Healthy Adult Opportunity
This week, our In Focus section comes from HMA Medicaid Market Solutions (MMS) Managing Director Matt Powers and Senior Consultant Desmond Banks. On January 30, 2020, the Centers for Medicare & Medicaid Services (CMS) convened an event titled, Transforming Medicaid: A New Opportunity for Better Health, in Washington, DC, during which CMS Administrator Seema Verma announced the Healthy Adult Opportunity (HAO), an optional Section 1115 Medicaid Demonstration initiative. Commonly referred to as, “block grant” or “spending cap” model, the HAO seeks to provide states with enhanced flexibility to design and administer parts of their Medicaid program. Administrator Verma articulated the HAO to be an important step to support the fiscal sustainability of Medicaid and invited state Medicaid directors to submit waiver applications.

Conservative states’ Medicaid expansion offers model for Missouri expansion
A new analysis of conservative state Medicaid expansion in Arkansas, Indiana and Ohio clarifies many of the questions raised about state-level costs and budget savings of a potential Missouri expansion. Researchers at ������ interviewed leaders directly involved with expansion in these states to evaluate the policy and operational adjustments they undertook to design a budget-conscious program while maximizing state value.

HMA prepares report detailing economic implications of a Medicaid expansion in Missouri
On January 30, 2020, the Missouri Hospital Association issued a press release outlining a report prepared by ������. .
The report, Medicaid Expansion in Missouri – Economic Implications for Missouri and Interviews Reflecting Arkansas, Indiana, and Ohio Experiences, was prepared by HMA MMS Managing Director Matt Powers and Managing Principal Sharon Silow-Carroll, and Jack Meyer. They conducted interviews with leaders directly involved with expansion in Arkansas, Indiana, and Ohio to evaluate the policy and operational adjustments they undertook to design a budget-conscious program while maximizing state value. Those interviews allowed clarification of many of the questions raised about state-level costs and budget savings of a potential Missouri expansion.
The report was commissioned by the Missouri Hospital Association and Missouri Primary Care Association and released in partnership with stakeholders from the healthcare community.

DC and Kentucky Medicaid Managed Care RFPs
This week, our In Focus section reviews two Medicaid managed care requests for proposals (RFPs) released on January 10, 2020. The District of Columbia Department of Health Care Finance (DHCF) issued an RFP for the DC Healthy Families Program (DCHFP); the District of Columbia Healthcare Alliance Program (Alliance); and the Immigrant Children’s Program (ICP) as part of a broader effort to fully transition Medicaid to managed care over the next five years. The new contracts will cover approximately 224,000 lives. Meanwhile, the Kentucky Cabinet for Health and Family Services (CHFS), Department for Medicaid Services (DMS) released a statewide Medicaid managed care RFP to serve approximately 1.2 million lives. In December 2019, Kentucky announced that it will cancel and rebid the current Medicaid managed care contracts.

Texas STAR Kids – Dallas Service Area RFP
This week, our In Focus section reviews the Texas STAR Kids Medicaid Managed Care in the Dallas Service Area (SA) request for proposals (RFP) released by the Texas Health and Human Services Commission (HHSC) on December 13, 2019. The RFP comes after Children’s Medical Center, which covers approximately 9,000 members under the program, said it would be leaving the market. The contracts for the SA are worth approximately $500 million. Anthem/Amerigroup will remain in the Dallas SA and continue to provide services. STAR Kids provides Medicaid coverage to individuals with disabilities under age 21.

West Virginia releases Medicaid managed care RFP
This week, our In Focus section reviews the West Virginia Mountain Health Trust request for proposals (RFP) released by the West Virginia Department of Administration (DOA) for the Department for Health and Human Resources (DHHR) on December 17, 2019. Mountain Health Trust (MHT) is the statewide physical and behavioral Medicaid managed care program. West Virginia will award contracts, worth over $1.5 billion, to three managed care organizations (MCOs), with implementation beginning July 1, 2020.

Michigan Medicaid Managed Care Results Announced
In previous editions of The Michigan Update (most recently in August) we have reported on the Michigan Department of Health and Human Services’ (MDHHS) release of a Request for Proposals (RFP) to re-procure its Medicaid managed care contracts. The RFP was released in early May with bidder responses due in early August. This procurement is for at least five years, with the possibility of up to three one-year extensions. The total cost of the procurement for five years is estimated to be $35 billion. On October 13, 2015 the State of Michigan announced the much anticipated results of the re-procurement.
Since the prices paid to the contracted HMOs are set by the state, the health plan selection was based solely on technical scores. The HMOs were required to bid on entire regions, which were configured differently than in the past. The reconfiguration required a number of the HMOs to expand their service areas to meet the “entire region” requirement. The new regional configuration appears in the map below:
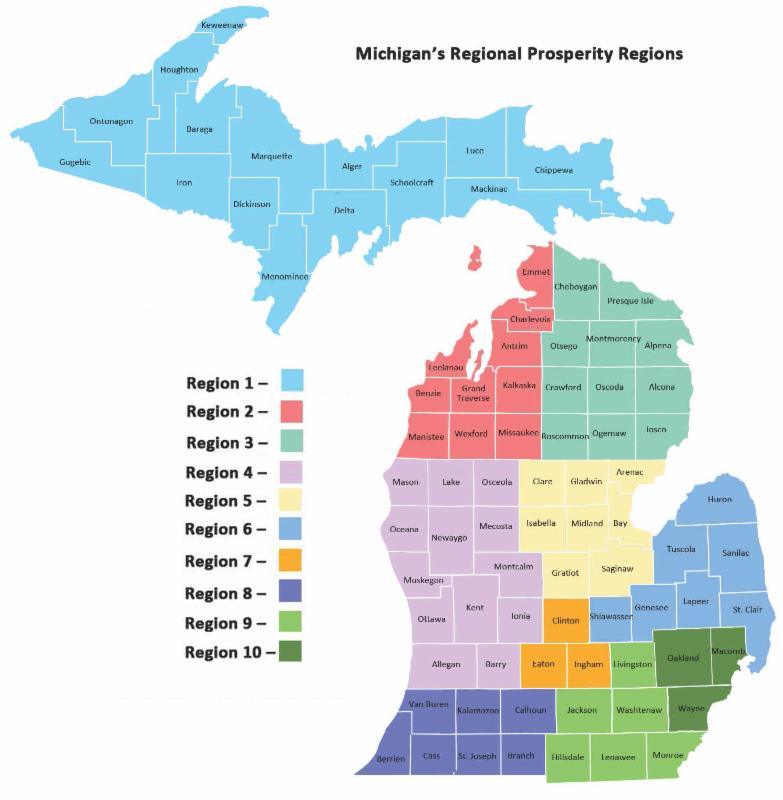
Note: Region 2 and Region 3 were required to be bid together.
The RFP included a proposed number of HMOs that would be awarded contracts for each of these regions. To minimize disruptions for Medicaid enrollees, in each region (other than the Upper Peninsula) the number of plans selected was one more than the proposed maximum number of awards for that region. Proposals from the HMOs were evaluated based on demonstrated competencies and also statements of their proposed approaches to many new initiatives related to population health, care management, behavioral health integration, patient-centered medical homes, health information technology and payment reform.
Not every HMO was successful in each region for which it submitted a bid. Two plans were not successful in any region. One is Sparrow PHP, which is an incumbent plan in Region 7. The other is MI Complete Health (Centene/Fidelis SecureCare) which is not currently a Medicaid plan in any part of the state but does have an Integrated Care Organization contract to serve dual Medicare/Medicaid enrollees in Macomb and Wayne counties as part of Michigan’s dual eligible demonstration.
The following table indicates the regions for which each bidding HMO was and was not successful. In addition, the numerical values show the rank of that plan based on their evaluation scores among the successful bidders for each region. If an HMO is a current contractor for all counties in a region, their result is shaded green. If the HMO is a current contractor for some but not all counties in a region, their result is shaded yellow. The number of Medicaid enrollees currently served in each of the regions, eligible through both “traditional” Medicaid and the Healthy Michigan Plan, appear in the bottom row on the table; across all regions, this is more than 1.6 million Medicaid enrollees.
Technical Evaluation Results
|
|
Region 1
|
Region 2
|
Region 3
|
Region 4
|
Region 5
|
Region 6
| Region 6 |
Region 8
|
Region 9
|
Region 10
|
|
Aetna Better Health
(CoventryCares)
|
|
|
|
|
No
|
|
|
Yes – 4
|
Yes – 4
|
Yes – 7
|
|
Blue Cross Complete
|
|
|
|
Yes – 3
|
|
Yes – 5
|
Yes – 3
|
|
Yes – 3
|
Yes – 5
|
|
HAP Midwest Health Plan
|
|
|
|
|
|
Yes – 6
|
|
|
No
|
No
|
|
Harbor Health
Plan
|
|
|
|
|
|
|
|
|
|
Yes – 8
|
|
McLaren Health
Plan
|
|
Yes – 3
|
Yes – 3
|
Yes – 4
|
Yes – 3
|
Yes – 3
|
Yes – 2
|
Yes – 3
|
Yes – 6
|
Yes – 4
|
|
Meridian Health Plan of MI
|
|
Yes – 1
|
Yes – 4
|
Yes – 5
|
Yes – 2
|
Yes – 4
|
No
|
Yes – 5
|
Yes – 5
|
Yes – 3
|
|
MI Complete Health
(Centene/Fidelis)
|
|
|
|
|
|
|
|
|
No
|
No
|
|
Molina Healthcare
of MI
|
|
Yes – 4
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
|
Priority Health Choice
|
|
No
|
No
|